Cryopreservation has marked a before and after in reproductive medicine. Thanks to advances in laboratory techniques, today it is possible to preserve reproductive cells and embryos for years while keeping their implantation potential intact. When the time comes to try for a pregnancy using these preserved resources, it is completely natural for doubts to arise about the technical and clinical procedures that are carried out.
In assisted reproduction consultations, one of the most frequent concerns of patients is understanding exactly what happens in the laboratory. Just as many women seek information on how to thaw eggs after a fertility preservation treatment, those couples or patients who have cryopreserved embryos from a previous In Vitro Fertilization (IVF) cycle want to know step by step how their future embryos come back to cellular life.
Throughout this article, we will explain objectively and in detail what the embryo devitrification process consists of, which is essentially embryo warming, as well as how the woman’s body is prepared to receive the embryo and what factors influence the success of the treatment.
Table of Contents
ToggleWhat is embryo warming (devitrification)?
Although colloquially we use the terms “freezing” and “thawing”, in modern assisted reproduction the technique used is called vitrification and devitrification.
The fundamental difference lies in the speed of the temperature change. Traditional freezing allowed the formation of small ice crystals inside the cells, which could damage their internal structures. Vitrification, on the other hand, is an ultra-fast cooling (down to -196 ºC) using substances called cryoprotectants. When performing the reverse process (devitrification or embryo warming), the embryo goes from a solid glass-like state to recovering its biological temperature (37 ºC) in a matter of seconds, avoiding any cellular damage.
Similarities and differences: egg warming vs. embryo warming
On a technical level, when embryologists consider how to warm eggs or how to perform embryo warming, the laboratory protocol they follow is practically identical.
The main difference lies in the biology of the cell itself. An egg is a single, large cell with a high water content, which historically made its survival more complex. An embryo, depending on the day of development in which it was vitrified (for example, in the blastocyst stage on day 5), is a set of multiple cells. Thanks to current culture media and cryoprotectants, both processes offer excellent survival rates.
The step-by-step process in the laboratory
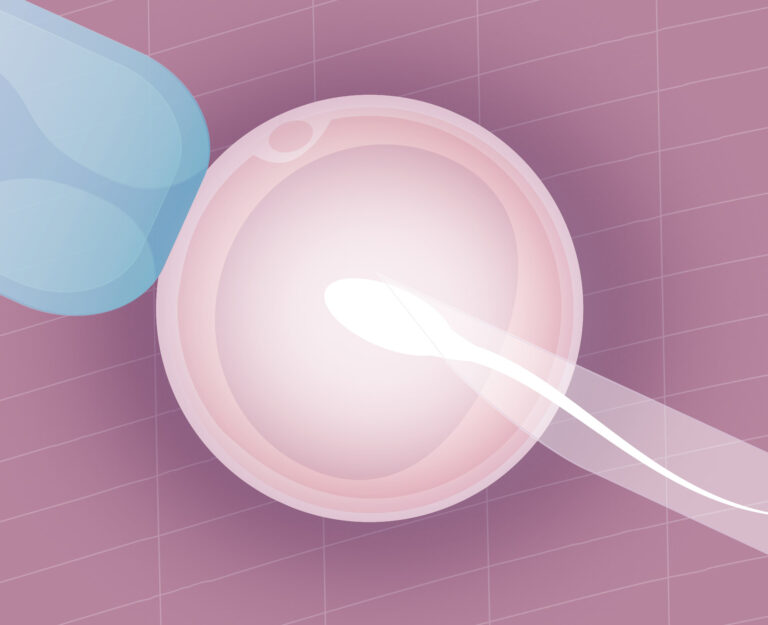
Work in the embryology laboratory requires microscopic precision. The embryo warming process is carried out on the same day the embryo transfer to the maternal uterus is scheduled and consists of the following steps:
- Strict identification: The support (a small straw) where the embryo is stored in the liquid nitrogen tanks is located, verifying the patients’ identity multiple times.
- Ultra-fast warming: The straw is removed from the liquid nitrogen (-196 ºC) and immediately immersed in a culture medium at 37 ºC. This drastic change is key to cellular survival.
- Cryoprotectant washing: The embryo is passed through different culture dishes with decreasing concentrations of special media. The goal is to extract the cryoprotectant substances from its cells that were used to freeze it and to rehydrate it progressively.
- Viability assessment: After a resting period in the incubator (usually between 2 and 4 hours), embryologists evaluate the embryo morphologically under the microscope to confirm that it has survived the process and that its cells have resumed their normal activity.
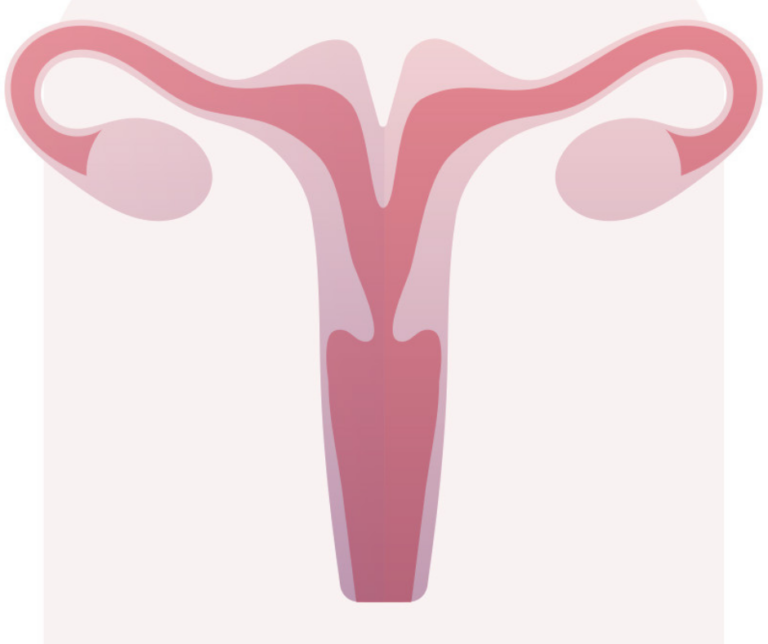
Endometrial preparation: the patient’s role
While the laboratory plans the embryo warming, the gynecological team focuses on preparing the “nest” that will host the embryo: the patient’s endometrium. This process is called endometrial preparation and can be done in two main ways:
- Natural cycle: The woman’s natural menstrual cycle is used, monitoring the growth of her own follicle and the thickness of the endometrium through ultrasounds. It is usually indicated for women with very regular periods.
- Substituted cycle: Hormonal medications (estrogen and progesterone) are administered to mimic the natural cycle and ensure the endometrium reaches the optimal thickness and trilaminar appearance for implantation.
It is important to consult with a specialized medical team to determine which type of endometrial preparation is most suitable based on the patient’s medical history.
Survival and success probabilities after embryo warming
The introduction of vitrification has brought about a paradigm shift. Currently, embryo survival rates after embryo warming exceed 90-95% in most high-quality laboratories.
This means that, in the vast majority of cases, the embryo survives intact and retains exactly the same implantation potential it had at the time it was vitrified. Transferring frozen embryos (what we know as cryotransfer) today offers clinical success rates comparable, and even in some contexts superior, to those of fresh embryo transfers, since it allows the process to be carried out in a cycle in which the woman’s body is not subjected to the hormonal stress of ovarian stimulation.
Frequently Asked Questions (FAQ)
Is the process painful for the patient? Not at all. The embryo warming process is carried out entirely in the laboratory. For the patient, the only clinical step is the embryo transfer, which is a quick, outpatient, and completely painless procedure (similar to a routine pap smear), requiring neither anesthesia nor hospital admission.
How long does the complete treatment take? The warming process in the laboratory takes just a few minutes, followed by a few hours of observation in the incubator. However, for the patient, the prior endometrial preparation treatment usually lasts between 12 and 15 days from the start of the period until the day of the transfer.
What are the chances of pregnancy? The probabilities depend mainly on the woman’s age at the time the embryo was generated and vitrified, as well as its morphological or genetic quality. As we mentioned, the vitrification technique guarantees that the embryo does not lose quality during the time it remains frozen.
When to consult a specialist? If you have vitrified embryos at your clinic and wish to try for a new pregnancy, you can request an appointment at any time. If you are experiencing difficulties conceiving naturally after a year of trying (or six months if you are over 35), it is time to have an initial medical consultation.
Conclusion
Understanding the science behind assisted reproduction, from knowing how to devitrify eggs to knowing the meticulous care we put into embryo warming, helps reduce uncertainty and face the treatment with greater peace of mind.
Current vitrification technology is extremely safe and effective. The transition from a state of cryopreservation to biological reactivation is a routine and highly standardized procedure in embryology laboratories, ensuring that your embryos have the highest chances of resulting in a healthy, ongoing pregnancy.
Remember that this article has an educational and informative purpose. Each case must be evaluated individually by a specialist to establish the diagnosis and the most appropriate medical protocol.
Bibliography and reference sources
To guarantee the medical rigor of this article, the information has been cross-referenced with publications and clinical guidelines from the most relevant institutions in the field of human reproduction:
- Spanish Fertility Society (SEF): Clinical practice guidelines on oocyte and embryo vitrification, and protocols for cryopreserved embryo transfer. (sefertilidad.net)
- European Society of Human Reproduction and Embryology (ESHRE): Consensus on good practices in In Vitro Fertilization (IVF) laboratories and cryobiology. (eshre.eu)
- American Society for Reproductive Medicine (ASRM): Recommendations on embryo cryopreservation and endometrial preparation for deferred transfer cycles. (asrm.org)